Orthotopic Models – Realistic Tumor Microenvironments
Orthotopic models mimic the human disease state more accurately than subcutaneous models by implanting tumor cells or tissue directly into the organ of origin. This preserves the tumor’s interaction with local stroma, vasculature, and immune environment, making these models essential for studying invasion, metastasis, and drug response in a clinically relevant setting.
Why choose orthotopic models?
- Organ-specific tumor growth: Captures tissue- and site-specific drug responses
- Natural metastatic behavior: Enables observation of spontaneous or distant-site metastasis
- Higher predictive value: Better recapitulates clinical efficacy vs. subcutaneous or cell-line-only models
- Real-time tumor tracking: Bioluminescence and fluorescence imaging for dynamic monitoring of progression and response
- Supports rare & aggressive cancers: Includes brain metastases, hematologic malignancies, and pretreated tumors
At LIDE, we offer orthotopic models built on PDX, CDX, and hematological tumors, across a wide spectrum of solid and liquid cancers.
Summary of available orthotopic PDX models
Leveraging our best-in-class PDX library, LIDE provides well-characterized orthotopic PDX models—each using luciferase-labeled tumor cells for non-invasive monitoring.
| Clinical Diagnosis | Gender | Age | PDX Pathology | Model ID |
|---|---|---|---|---|
| DLBCL | F | 42 | Diffuse Large B cell Lymphoma | LD1-0026-410827 |
| Refractory Multiple Myeloma | M | 54 | Multiple Myeloma | LD1-0029-361847 |
| Brain metastasis of breast cancer | F | 64 | Breast cancer with brain metastases | LD1-2009-362541 |
| Triple-negative breast cancer | F | 38 | Poorly differentiated adenocarcinoma | LD1-2009-362263 |
| AML-M4/5 | F | 38 | Not specified | LD1-0040-361280 |
| AML-M5 | M | 23 | High-grade lymphoma/leukemia | LD1-0040-362349 |
| AML-M2 | F | 57 | High-grade lymphoma/leukemia | LD1-0040-362393 |
Analysis and Readouts:
- IVIS bioluminescent imaging for real-time tracking
- FACS and molecular profiling for endpoint validation
- Tumor burden, survival, and toxicity assessment
Summary of available orthotopic CDX models
When patient tissue isn’t available or preferred, LIDE provides well-characterized orthotopic CDX models across multiple organs and tumor types.
| Indication | Cell Line | Implantation Site | SOC Example |
|---|---|---|---|
| Glioblastoma | U-87MG-luc, LN229-luc, U251-luc | Brain cortex (stereotactic) | Temozolomide |
| Lung Adenocarcinoma | A549-luc (orthotopic & metastatic) | Lung lobe / lateral vein | Trametinib |
| Colorectal Cancer | HCT116-luc | Cecum wall | |
| Hepatocellular Carcinoma | Hep 3B-luc | Liver parenchyma | |
| Pancreatic Cancer | PANC-1-luc | Pancreas | Gemcitabine |
| Breast Cancer (TNBC) | MDA-MB-231-luc | Mammary fat pad | Gemcitabine |
| Prostate Cancer | LNCaP FGC-luc, PC-3-luc | Dorsal lobe of prostate | Docetaxel |
| Bladder Cancer | SW780-luc, RT112-luc | SW780: (unspecified); RT112: Detrusor & mucosa | SW780: Docetaxel; RT112: Sunitinib |
| Leukemia & Lymphoma | MV4-11-luc, NALM6-luc, K-562-luc, Raji-luc | Systemic (lateral vein) | Sunitinib |
| Murine Models | GL261-luc, Hepa1-6-luc, H22-luc | Brain / Liver | Temozolomide, Sorafenib, anti-PD-1, mPD-1 |
Benefits of using orthotopic CDX Models:
- Enables rapid proof-of-concept and dose-response studies
- Supports mechanism-of-action and metastasis tracking
- Scalable and reproducible: ideal for early screening or validation before PDX scale-up
Model Customization Available:
If your study requires a specific indication, strain, or delivery route, LIDE’s scientific team can support custom orthotopic development on request.
Featured Studies
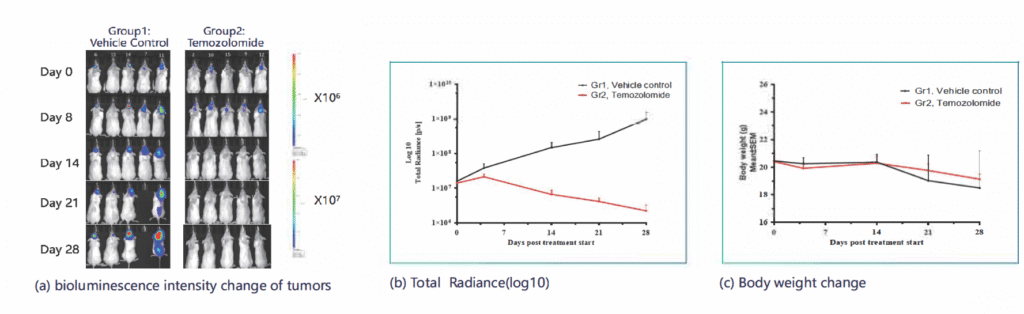
- Tumor implanted in the brain cortex via stereotactic injection
- Assessed response to Temozolomide
- Results: Significant inhibition of tumor progression and metastasis to the spine; monitored via BLI and confirmed through post-mortem analysis
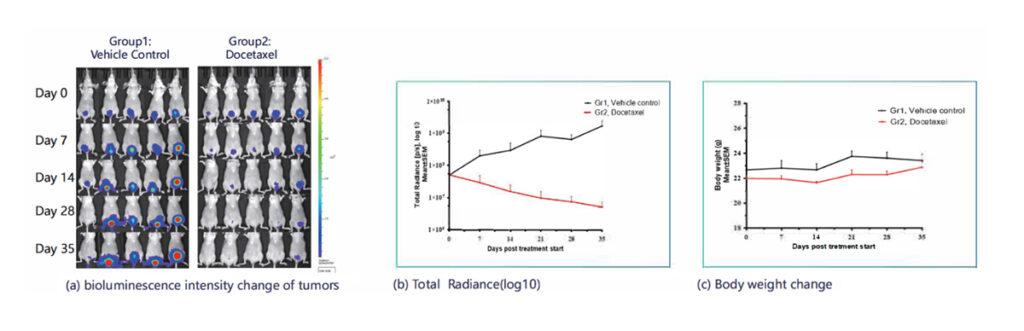
- Tumor implanted into the bladder mucosa using catheter-based delivery
- Treated with Docetaxel
- Results: Reduced tumor radiance and stabilized body weight, confirming therapeutic efficacy
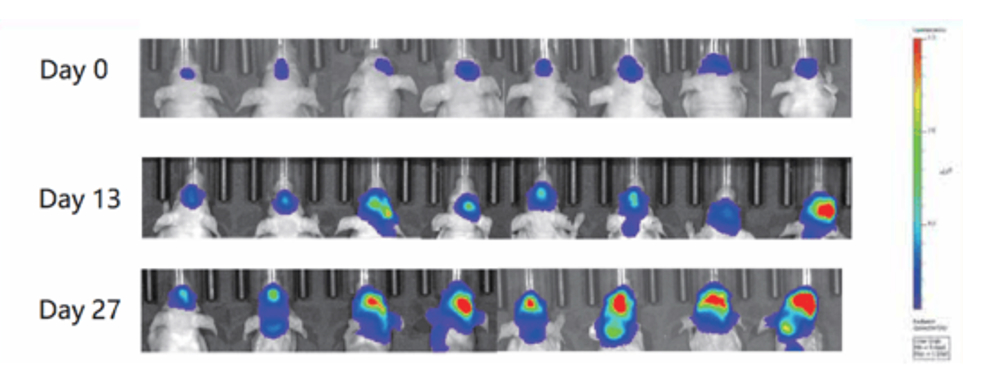
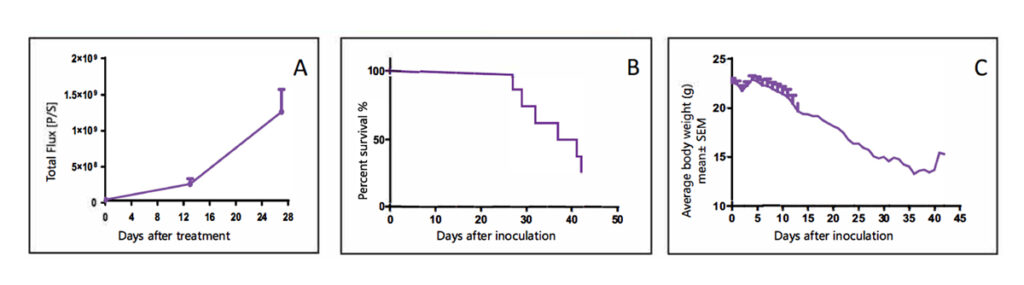
- Method: Tumor cells derived from PDX tumors are labeled with luciferase and implanted into the mouse brain via stereotactic injection.
- Endpoints: Tumor growth (via BLI), survival curves, and body weight changes.
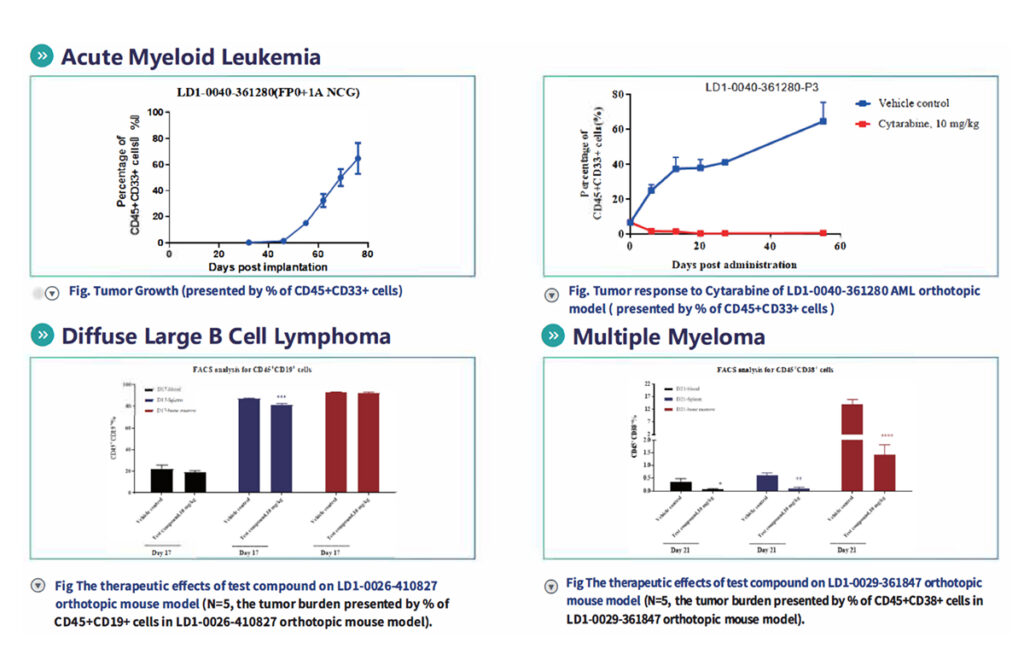
- Use Case: Hematologic malignancies (e.g., AML, DLBCL, Multiple Myeloma).
- Method: PDX-derived cells are implanted into immunodeficient mice intrafemorally or intravenously after preconditioning.
- Endpoints: Flow cytometry (FACS) tracking of tumor burden via specific immune cell markers (e.g., CD45+, CD33+, CD19+, CD38+).